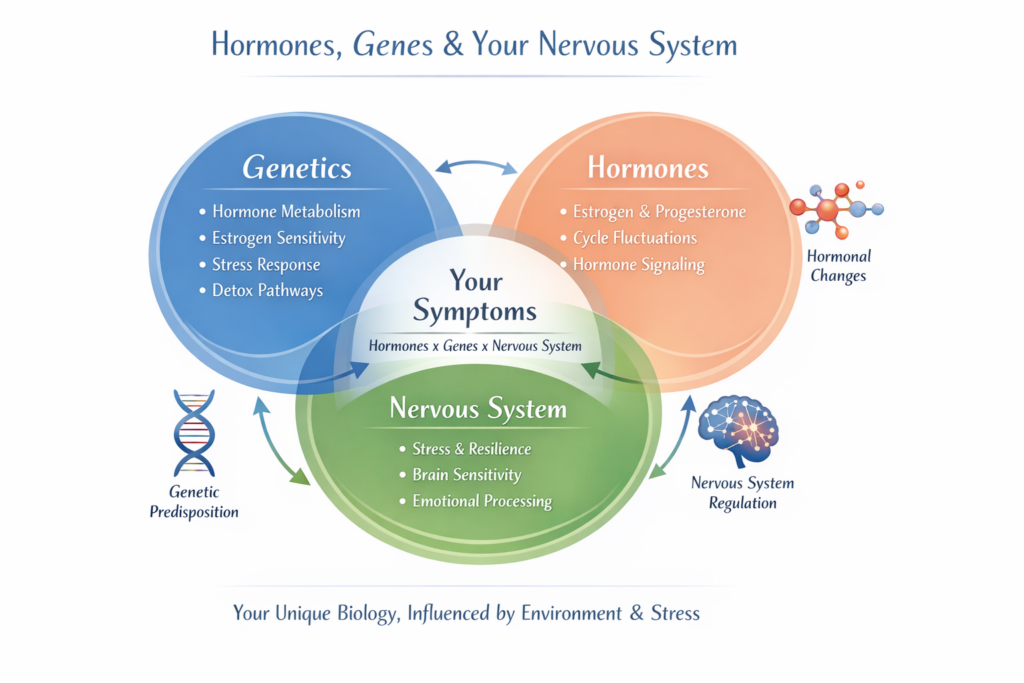
Hormones, the Nervous System, and Your Unique Genetic Sensitivity
Many women reach a point where they’ve done “everything right.”
They’ve had blood work.
They’ve been told their hormones are normal.
And yet—month to month—their symptoms change.
Some cycles feel manageable.
Others feel heavy, anxious, foggy, or emotionally intense.
This disconnect can be deeply frustrating and invalidating.
The missing piece is often how hormones are communicated, interpreted, and regulated—not just how much of them are present.
Hormones Are Signals—The Nervous System Is the Interpreter
Hormones do not act on their own.
They are chemical messages sent throughout the body.
The nervous system—especially the brain—is what receives those messages and decides how strongly they are felt.
This means:
- Hormone levels can be similar from one month to the next
- But your experience of those hormones can be very different
Why? Because interpretation matters.
Stress Changes Hormone Perception—Not Just Hormone Levels
When the nervous system is under stress (emotional, mental, physical, or cumulative), it becomes more reactive.
This can:
- Amplify sensitivity to estrogen or progesterone shifts
- Lower tolerance for normal hormonal fluctuations
- Increase symptoms like anxiety, sleep disruption, irritability, or overwhelm
In this state, even “normal” hormone changes can feel intense.
This is why symptoms often worsen during:
- High responsibility periods
- Ongoing emotional load
- Poor sleep phases
- Life transitions—even positive ones
The body isn’t malfunctioning.
It’s responding.
Where Genetics Enters the Picture
Genetics helps explain why two women can have similar hormones and feel completely different.
Your genes influence:
- How hormones are produced
- How quickly they are broken down
- How efficiently they are cleared
- How sensitive your brain and tissues are to hormonal shifts
- How strongly your nervous system reacts to stress
Some women are genetically wired to be:
- More sensitive to estrogen fluctuations
- Slower to clear hormones
- More reactive to stress signals
- More prone to nervous system activation
None of this is good or bad—it’s information.
Genetics doesn’t determine your fate, but it shapes your hormonal experience.
Why Symptoms Change From Month to Month
Your cycle doesn’t start from zero each month.
It carries forward:
- Last month’s stress load
- Sleep quality
- Emotional processing
- Inflammation levels
- Nervous system tone
If the nervous system enters a cycle already overstimulated or depleted, hormone shifts may feel sharper—even if hormone levels themselves haven’t changed dramatically.
This is especially noticeable in perimenopause, when:
- Ovulation is less consistent
- Progesterone support may be lower
- Estrogen fluctuations are more pronounced
In this context, the nervous system becomes a key regulator of symptoms.
Why Labs Can Look “Normal” and Still Miss the Story
Hormone tests typically show:
- A single moment in time
- One point in a moving rhythm
They don’t capture:
- Rapid fluctuations
- Nervous system sensitivity
- Genetic metabolism differences
- How stress or sleep affected hormone signaling that month
Symptoms often reflect communication quality, not just hormone quantity.
Nervous System Regulation: The Missing Foundation
For many women, stabilizing symptoms isn’t about forcing hormones into balance—it’s about supporting regulation.
When the nervous system feels safer and more resourced:
- Hormone signals are perceived more gently
- Fluctuations feel less disruptive
- Resilience improves—even when cycles vary
This is why approaches that support:
- Stress regulation
- Emotional processing
- Sleep quality
- Digestive and metabolic stability
often improve hormonal symptoms—even without changing hormone levels directly.
A More Compassionate Way to Understand Symptoms
Instead of asking:
“Why am I so inconsistent?”
A more helpful question is:
“What is my system responding to right now—and how can I support it?”
Symptoms are not random.
They are contextual.
Empowerment: What This Means for You
Understanding hormones through the lens of:
- Nervous system regulation
- Genetic sensitivity
- Whole-body communication
allows for:
- Personalized support instead of generic protocols
- Less self-blame
- More clarity and trust in your body
Your body isn’t unpredictable—it’s responsive.
A Gentle Invitation
If your symptoms shift from month to month, it doesn’t mean something is wrong with you.
It means your body is communicating—and learning how to listen can change everything.
🌿
Scientific References:
Key References (Mapped to Claims)
Hormones are signals interpreted by the nervous system
- McEwen BS.
Protective and damaging effects of stress mediators.
N Engl J Med. 1998;338(3):171–179.
https://doi.org/10.1056/NEJM199801153380307 - McEwen BS, Akil H.
Revisiting the stress concept: implications for affective disorders.
J Neurosci. 2020;40(1):12–21.
https://doi.org/10.1523/JNEUROSCI.0733-19.2019
Stress changes hormone sensitivity, not just output
- Young EA et al.
Hormones and mood: stress sensitivity and HPA–HPG interaction.
Biol Psychiatry. 2000;48(9):843–851.
https://doi.org/10.1016/S0006-3223(00)00968-2
Genetics influence hormone metabolism & sensitivity
- Zhu BT, Conney AH.
Functional role of estrogen metabolism in target tissues.
Endocr Rev. 1998;19(4):463–494.
https://doi.org/10.1210/edrv.19.4.0335 - Raftogianis R et al.
Estrogen metabolism and conjugation pathways.
Drug Metab Dispos. 2000;28(12):1517–1523. - Payne JL et al.
Genetic vulnerability to hormone-related mood disorders.
Biol Psychiatry. 2007;61(7):831–839.
https://doi.org/10.1016/j.biopsych.2006.06.028
Perimenopause & nervous system sensitivity
- Schmidt PJ et al.
Estrogen withdrawal and mood in perimenopause.
Am J Psychiatry. 2015;172(4):366–375.
https://doi.org/10.1176/appi.ajp.2014.14070818 - Gordon JL et al.
Neurobiological underpinnings of perimenopausal mood changes.
Menopause. 2016;23(7):784–793.
https://doi.org/10.1097/GME.0000000000000622


