One month you feel steady, clear, and grounded.
The next month—same cycle timing, same lifestyle—everything feels off.
Sleep is lighter. Emotions are closer to the surface. Your body feels unfamiliar.
And the question arises:
“Why does this keep changing?”
For many women, this variability is more distressing than the symptoms themselves. Not knowing what to expect can create self-doubt, frustration, and even fear that something is “wrong.”
The truth is much more reassuring.
Your Hormones Are Communicating—Not Operating on a Fixed Schedule
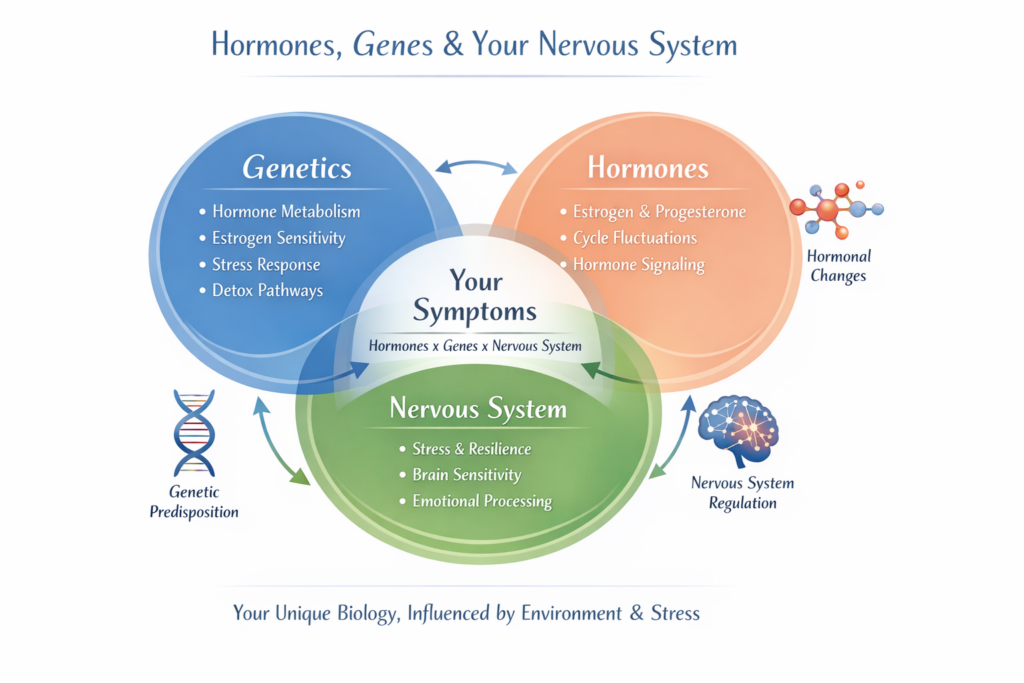
Hormones don’t act in isolation. They are part of a dynamic communication network involving:
- The brain
- The ovaries
- The nervous system
- The immune system
- The digestive and detoxification systems
This communication is responsive, not rigid.
That means your cycle is influenced not only by where you are hormonally—but by what your body is experiencing.
Why Symptoms Can Shift From One Cycle to the Next
1. Hormone Signaling Is Sensitive to Stress
Stress doesn’t just “affect cortisol.”
It changes how the brain communicates with the ovaries and how tissues perceive hormone signals.
Even when hormone levels are similar on paper, your nervous system may interpret them differently depending on:
- Emotional load
- Mental fatigue
- Ongoing pressure or unresolved stress
This can shift symptoms such as anxiety, sleep disruption, PMS, or low resilience—sometimes dramatically.
2. Sleep Changes Hormone Reception
Sleep is not just restorative—it is regulatory.
Poor or fragmented sleep can:
- Alter estrogen and progesterone signaling
- Increase sensitivity to hormone fluctuations
- Amplify nervous system reactivity
This helps explain why one cycle feels manageable and the next feels overwhelming—despite “nothing obvious” changing.
3. Nutrition Influences Hormone Processing, Not Just Levels
Hormones must be:
- Produced
- Transported
- Metabolized
- Cleared
Nutrient availability affects every step of this process.
Changes in:
- Protein intake
- Blood sugar stability
- Digestive function
- Liver detox capacity
can subtly shift how hormones move through the body—altering symptoms from month to month.
4. Life Changes Leave Hormonal Imprints
Your body doesn’t reset at the start of each cycle.
Life events—whether joyful or challenging—leave physiological traces:
- Travel
- Illness
- Emotional stress
- Increased responsibility
- Grief, transitions, or uncertainty
These experiences influence hormone communication long after the event itself has passed.
Why This Is Especially Noticeable in Perimenopause
In perimenopause, ovulation becomes less predictable.
This changes progesterone availability and increases estrogen variability.
When baseline hormone rhythms are already shifting, the system becomes more sensitive to external inputs like stress, sleep, and emotional load.
This is why many women say:
“I don’t recognize my patterns anymore.”
Nothing is broken.
Your system is adapting.
A More Helpful Question to Ask
Instead of asking:
“What’s wrong this month?”
Try asking:
“What might my body be responding to right now?”
This reframes symptoms as information, not failure.
Empowerment: What Helps Stabilize Month-to-Month Experience
The goal is not to force consistency—but to support resilience.
Helpful foundations include:
- Supporting nervous system regulation
- Protecting sleep rhythms
- Stabilizing blood sugar
- Reducing unnecessary physiological stress
- Understanding your unique hormonal sensitivity
When the system feels supported, hormonal fluctuations are often experienced more gently, even if they still occur.
An Invitation
If your symptoms feel unpredictable, it doesn’t mean your body is unreliable.
It means your body is responsive.
Understanding that responsiveness is the first step toward working with your cycle instead of feeling at its mercy.
________________________________________________________________________________________
References:
Core Claims Supported
- Hormone signaling is dynamic and responsive
- Stress alters HPO-axis communication
- Sleep disruption affects hormone regulation
- Nutrition influences hormone metabolism
- Perimenopause increases variability rather than linear decline
Key References (Mapped to Claims)
Hormone communication is dynamic, not static
- Veldhuis JD et al.
Pulsatile hormone secretion and its physiological regulation.
Endocr Rev. 2008;29(7):823–864.
https://doi.org/10.1210/er.2008-0012
Stress alters reproductive hormone signaling
- Berga SL, Loucks TL.
The diagnosis and treatment of stress-induced anovulation.
Minerva Ginecol. 2006;58(1):45–54. - Tilbrook AJ et al.
Stress and reproduction: central mechanisms.
Endocr Rev. 2000;21(2):182–204.
https://doi.org/10.1210/edrv.21.2.0392
Sleep disruption affects hormonal regulation
- Leproult R, Van Cauter E.
Effect of sleep loss on neuroendocrine function.
Lancet. 2010;354(9188):1435–1439.
https://doi.org/10.1016/S0140-6736(99)01376-8 - Gold EB et al.
Relation of sleep disturbance to perimenopausal symptoms.
Am J Epidemiol. 2004;160(4):331–340.
https://doi.org/10.1093/aje/kwh228
Nutrition & metabolism influence hormone processing
- Rothman MS, Wierman ME.
How nutrition influences reproductive function.
Endocrinol Metab Clin North Am. 2007;36(1):187–205.
https://doi.org/10.1016/j.ecl.2006.11.003 - Michalakis K et al.
Diet, insulin resistance, and reproductive hormones.
Hum Reprod Update. 2013;19(1):70–89.
https://doi.org/10.1093/humupd/dms034
Perimenopause = fluctuation, not smooth decline
- Hale GE, Burger HG.
Hormonal changes in perimenopause.
Endocr Rev. 2009;30(1):76–131.
https://doi.org/10.1210/er.2008-0019 - Santoro N et al.
Characterization of reproductive hormonal dynamics in the menopausal transition.
J Clin Endocrinol Metab. 1996;81(4):1495–1501.
https://doi.org/10.1210/jcem.81.4.8636358





