Why things feel different—and why that makes sense
Perimenopause is the transition phase before menopause. It often begins years before periods stop completely, sometimes as early as the late 30s or early 40s. During this time, your hormones are not simply “declining”—they are fluctuating and changing their rhythm.
Understanding what’s happening hormonally can bring clarity, reassurance, and a sense of control.
What Changes in Perimenopause?
In a typical reproductive cycle, hormones follow a fairly predictable pattern.
In perimenopause, that pattern becomes less consistent.
The key change is not estrogen alone—it is irregular ovulation, which affects how all hormones interact.
The Four Key Hormones in Perimenopause
🌱 FSH – Follicle Stimulating Hormone
The brain trying harder
FSH is produced by the brain to signal the ovaries to mature an egg.
In perimenopause:
- The ovaries respond less consistently
- The brain increases FSH to “turn up the signal”
- FSH levels may rise earlier or fluctuate widely
What this can feel like:
Irregular cycles, skipped periods, or cycles that suddenly shorten or lengthen.
🌸 Estradiol (Estrogen)
Fluctuating, not disappearing
Estradiol does not decline smoothly in perimenopause.
Instead:
- Some cycles have very high estrogen
- Other cycles have very low estrogen
- The swings can be more intense than earlier in life
What this can feel like:
- Mood changes or anxiety
- Breast tenderness
- Headaches
- Hot flashes or night sweats (especially when estrogen drops suddenly)
- Feeling great one month and depleted the next
This unpredictability is one of the most confusing aspects of perimenopause.
🔔 LH – Luteinizing Hormone
The inconsistent ovulation signal
LH is responsible for triggering ovulation.
In perimenopause:
- LH surges may be weaker or mistimed
- Ovulation may not occur every cycle
When ovulation doesn’t happen, the hormonal sequence that normally follows is interrupted.
🌙 Progesterone
The most affected hormone
Progesterone is produced only after ovulation.
In perimenopause:
- Fewer ovulatory cycles → less progesterone
- Progesterone levels become inconsistent or low
What this can feel like:
- Increased anxiety or feeling “wired but tired”
- Sleep disruption or early waking
- PMS that feels stronger or lasts longer
- Heavier or more symptomatic periods
For many women, progesterone-related symptoms appear before estrogen-related ones.
How the Perimenopausal Cycle Often Looks
Instead of a smooth rhythm, many cycles follow this pattern:
- Estrogen rises (sometimes too much, sometimes not enough)
- Ovulation may or may not occur
- Progesterone support may be weak or absent
- Hormones drop abruptly → symptoms appear
This stop-and-start signaling explains why symptoms can feel chaotic rather than gradual.
“My Labs Are Normal—So Why Do I Feel This Way?”
This is one of the most common and frustrating experiences in perimenopause.
Hormone tests often:
- Capture a single moment, not the full pattern
- Miss rapid fluctuations
- Fall within “normal” ranges that don’t reflect individual sensitivity
Symptoms are often driven by hormonal shifts and nervous system response, not just absolute numbers.
Why Understanding This Matters
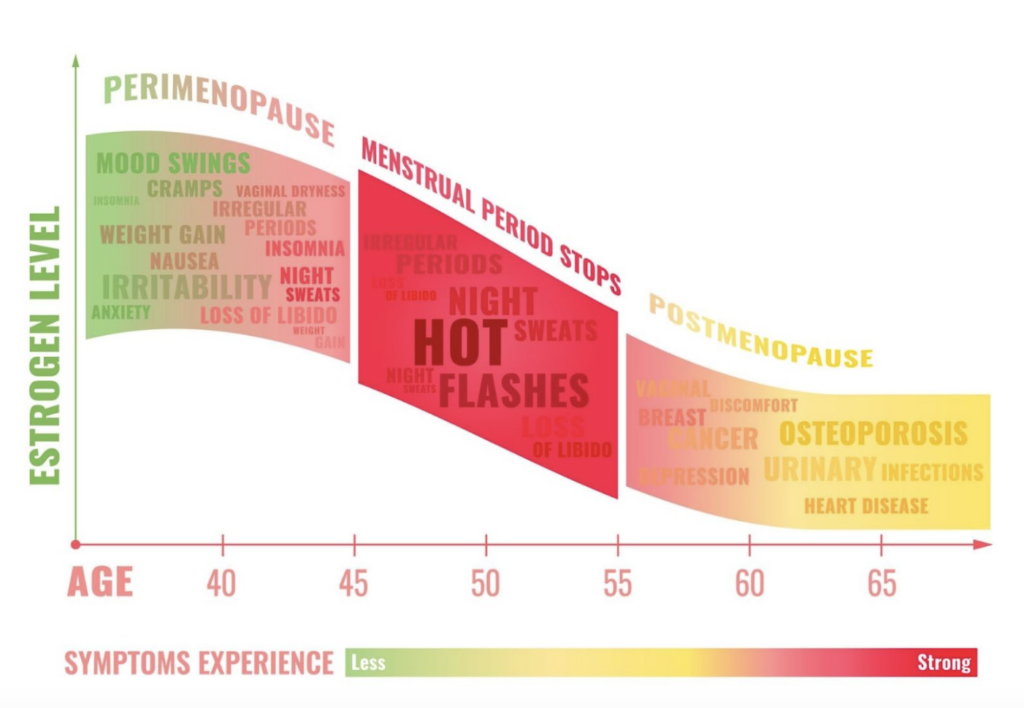
Perimenopause is not a failure of the body.
It is a neurological and hormonal transition.
Understanding what’s happening allows us to:
- Support the right hormone at the right time
- Focus on rhythm, resilience, and nervous system balance
- Reduce fear and self-blame
- Choose personalized, gentle strategies instead of guessing
An Invitation
If your cycle, mood, sleep, or energy no longer feel predictable—or if you feel “not quite like yourself anymore”—this may be your body moving through perimenopause.
Support during this phase can be informational, personalized, and empowering.
You don’t need to navigate it alone 🌿





